As students readjust to in-person learning in many schools this fall, states and school districts are implementing policies to prevent COVID-19 outbreaks and ensure the health of the children most disproportionately impacted by the pandemic, including those with special health care needs, from communities of color, and from lower income families. States are making a variety of decisions around COVID-19 immunizations in schools and determining which approaches to adopt to best serve their youth populations.
To date, 19 states have implemented laws and policies regarding school COVID-19 immunization mandates. Only two states (California and Illinois) require, based on state-level decisions, that students of a certain age are vaccinated to attend school. Many other states (17 states) have enacted bans on requiring COVID-19 vaccination as a condition of in-person learning. State progress in establishing and refining school immunization policies has coincided with advancing approval of the Pfizer/BioNTech COVID-19 vaccine for children. The Food and Drug Administration (FDA) issued an emergency use authorization (EUA) of the Pfizer COVID-19 vaccine for youth ages 12-15 in May and recently expanded authorization to children ages 5-11. As full capacity rollout of the Pfizer/BioNTech vaccine for younger children begins this week and pediatric COVID-19 cases fluctuate from an early September peak, state policies on COVID-19 vaccine mandates in schools continue to shift.
Vaccine Mandates
On October 1, California implemented the country’s first statewide COVID-19 vaccine mandate for K-12 students. Governor Gavin Newsom announced that the state will require all children attending in-person classes to be immunized against COVID-19. This requirement will go into effect at the beginning of the first term following full FDA approval of a vaccine for youth ages 5-11 and 12 and older. The California Department of Public Health will operationalize the measure by adding the COVID-19 vaccine to its list of immunizations required for public and private school attendance.
As authorization of the vaccine for children proceeds, more states may consider policies such as California’s mandate to address vaccine requirements in school-related settings. Officials in Hawaii and the District of Columbia recently required that high school students are vaccinated against COVID-19 in order to participate in school athletics. While only specific to institutions of higher education, Illinois Governor JB Pritzker issued an executive order requiring all public and private college students attending classes in-person to either receive the COVID-19 vaccine or undergo weekly testing. COVID-19 vaccine mandates, especially those pertaining to private businesses or hospitals, have often included similar testing opt-outs, reflecting the array of vaccine policy options. As of November 8, the vaccine mandates in California and Illinois are the only state-level actions requiring students to receive the COVID-19 vaccine for in-person school attendance.
While NASHP tracking remains focused on state-level policies, districts and schools have also started to enact local student vaccine mandates. Prior to Governor Newsom’s announcement, several large urban school districts in California, notably those in Los Angeles, Oakland, and Sacramento, voted that in-person students above age 12 must receive the COVID-19 vaccine. A handful of smaller cities across the country have announced similar measures. In actions resembling those of Hawaii and D.C., some northern Virginia school districts, including Fairfax County and Arlington County, are requiring COVID-19 vaccination for youth participating in high school athletics. Many institutions of higher education across the country have also decided, independently from state officials, to add the COVID-19 vaccine to their lists of required immunizations. For example, all public and private colleges in the state of Rhode Island determined that in-person students need to be vaccinated against COVID-19 for the fall semester. Additionally, public higher education or community college systems, such as those in Massachusetts, have mandated the COVID-19 vaccine for in-person classes without a state government-level policy to do so.
School staff are another population that states have considered in addressing school vaccine mandates. President Biden’s “Path out of the Pandemic Plan” unveiled in September requires staff in Head Start programs, Department of Defense schools, and Bureau of Indian Education schools to receive the COVID-19 vaccine. The plan also urges all states to adopt vaccine requirements for school employees. As of November 8, ten states and DC have implemented COVID-19 vaccine mandates for school staff, with nine requirements providing a testing opt out choice.
Bans on Vaccine Mandates
In efforts to prevent school vaccine mandates, 17 states, as of November 8, have adopted bans on requiring the COVID-19 immunization as a condition of in-person learning. These measures have largely been passed through state law (in 13 states) and the remainder through executive order (in four states). Among states with bans, there is significant variation in which categories of schools are restricted from pursuing mandates. For example, Alabama law prohibits “institutions of education,” broadly including public and private K-12 schools and colleges, from requiring the COVID-19 vaccine for attendance. In South Carolina, lawmakers included a restriction in the state’s budget appropriations law that prevents state-supported institutions of higher education (public universities) from using state funds to require student proof of COVID-19 vaccination.
FDA authorization of the COVID-19 vaccine is an additional factor distinguishing state bans. For example, Ohio law bars public schools and colleges from requiring students to receive vaccines that have yet to gain full FDA approval. According to this measure, Ohio schools can legally compel students 16 and older to receive the FDA approved Pfizer/BioNTech vaccine but are prohibited from adopting mandates for younger children while the vaccine is under EUA.
Challenges to State Actions
State strategies to address school vaccine mandates have undergone intense public and legal scrutiny. Amidst protests of California’s statewide student COVID-19 vaccine requirement, several lawsuits have been filed against the local-level mandates within the state, citing concerns about discrimination against childrens right to an education. An Oregon judge recently denied attempts to halt the states vaccine requirement for school staff, resolving just one of a litany of mandate-related legal actions in the state. Bans on mandates have also been challenged as an Arizona judge declared that state law prohibiting universities from requiring the COVID-19 vaccine was unconstitutional. These public concerns and legal proceedings around vaccine mandates and other school COVID-19 mitigation efforts have continued to proliferate as states adopt new policies. Legal considerations are impacting the debate around vaccine mandates in schools and may affect current and future state actions.
As the pandemic and vaccine approval progress, states will continue to advance and reformulate policies related to COVID-19 immunization requirements in schools. The NASHP Back to School landing page and tracker provide resources and continuous updates on state approaches to assist schools and support children returning to in-person learning.
Acknowledgments: This blog was supported by the Health Resources and Services Administration (HRSA) of the US Department of Health and Human Services (HHS) under grant number U2MOA39467 the National Organizations of State and Local Officials co-operative agreement. This information or content and conclusions are those of the authors and should not be construed as the official position or policy of, nor should any endorsements be inferred by HRSA, HHS or the US government.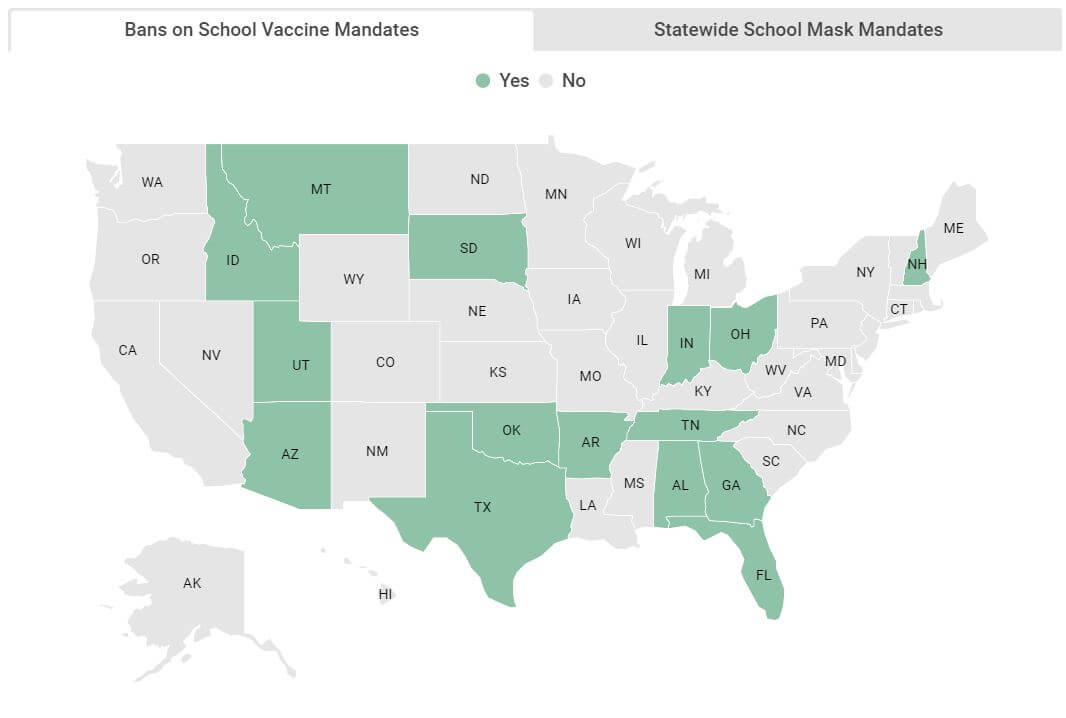 View Map/Chart on School Vaccine Mandates and Mask Mandates
View Map/Chart on School Vaccine Mandates and Mask Mandates




