Vaccination against Human Papillomavirus (HPV) continues to lag behind national benchmarks, leaving adolescents vulnerable to the development of preventable HPV-related cancers. The COVID-19 pandemic has had a tremendous negative impact upon these rates since 2020, as parents and healthcare providers have faced stay-at-home orders, disease surges, and a heavily burdened healthcare system. With nearly 80 million Americans — 1 in 4 — infected with HPV, getting HPV vaccinations back on track is critical to preventing future disease, suffering, and death. It is estimated that 35,000 new HPV-related cancers will be diagnosed this year. The vaccine, which has been recommended since 2006, can prevent more than 90% of those cancers when given at the recommended ages (American Cancer Society, 2022). This paper highlights several successful state initiatives that policymakers may consider adopting to improve routine HPV vaccination rates among adolescents and provide catch-up vaccinations to the estimated one million adolescents who are now behind due to the challenges of the pandemic.
Background
Early in the pandemic, as states issued stay-at-home orders, medical providers grappled with how to engage sick and well patients, schools shifted to remote learning, and parents faced new barriers to getting their children their routine childhood vaccinations. As a result, vaccination coverage rates plummeted, leaving many children vulnerable to preventable diseases. According to a report from the Centers for Disease Control and Prevention (CDC), administration of Human Papilloma Virus (HPV) vaccines to children ages 9-12 years and adolescents aged 13-17 years in 10 jurisdictions declined a median of 63.3 percent and 71.3 percent, respectively, during March-May 2020 compared with the same period in 2018 and 2019. While administration rates have improved, they have not been sufficient to catch up children who missed vaccinations in 2019. The American Academy of Pediatrics, the American College of Obstetricians and Gynecologists, the American Cancer Society, and the Advisory Committee on Immunization Practices (ACIP), among others, strongly recommend the administration of HPV vaccine in males and females to prevent several types of cancer, as the vaccine is proven safe and extremely effective. Although HPV is responsible for 70-90% of cervical and head and neck cancers in the U.S., vaccination rates remain lower than for other recommended childhood vaccinations.
According to Memorial Sloan Kettering Cancer Center, adolescents with public insurance have missed an estimated one million doses of HPV vaccine since March 2020. This amounts to a nearly 21 percent drop in vaccinations compared to March 2020, a time when vaccine uptake was already well below the Healthy People 2030 goal of getting 80 percent of adolescents aged 13 through 15 years vaccinated. According to America’s Health Rankings for 2020, the U.S. HPV vaccine coverage rate for adolescents aged 13 through 17 years was 54.2%.
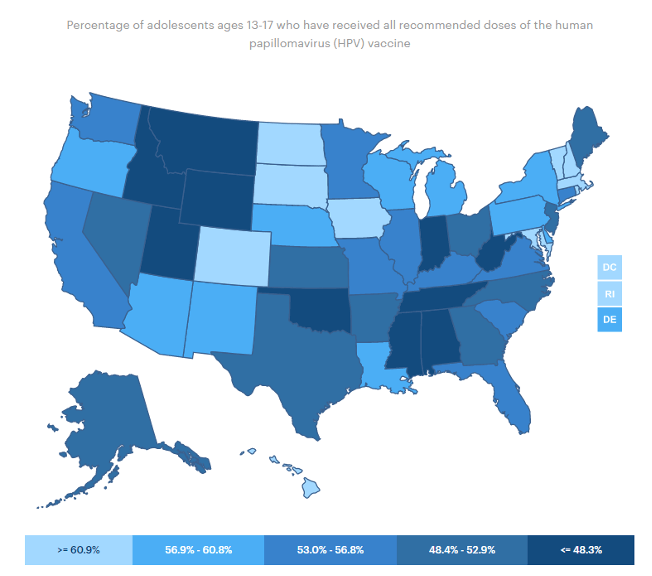
https://www.americashealthrankings.org/explore/annual/measure/Immunize_HPV/state/ALL
Challenges to vaccinating young people against HPV infections include lack of education around the cancer-preventing benefits of the vaccine; false beliefs that males are not at risk for HPV-related cancers; beliefs that only sexually active individuals can get HPV infections or that the vaccine causes children to become sexually active; and most recently, hesitancy to schedule preventive health visits out of fear of being exposed to SARS-CoV-2. Providers are also citing concern that lack of confidence in COVID-19 vaccines is beginning to influence acceptance of routine childhood vaccines.
State Strategies to Increase HPV Vaccine Uptake
States have developed several best practices for overcoming barriers to vaccination as they work to increase HPV vaccine uptake and improve the health of their residents. The list below includes several examples of such initiatives that state officials and policymakers may consider adopting when working to improve HPV vaccine coverage rates in their states.
Educate Medical Providers
Medical provider recommendations to receive HPV vaccines are highly correlated with improved vaccine uptake, yet poor HPV vaccine coverage rates indicate providers are missing opportunities to vaccinate their patients.
States can play an important role in educating healthcare providers on the importance of HPV vaccinations and how to communicate a strong recommendation to receive the vaccine to their patients. Prior to the pandemic, the North Dakota immunization program used Centers for Disease Control and Prevention (CDC) cooperative agreement funding to develop educational presentations that were delivered by trained peer content experts and public health professionals in clinics across the state. These presentations included information on HPV-related disease epidemiology, vaccine safety and efficacy, and evidence-based communication strategies for discussing immunizations. The program found that clinics that received the intervention had improved rates of HPV vaccination initiation and series completion as compared to clinics that did not receive the intervention and helped to move North Dakota to rank among states with the highest rates for up-to-date HPV vaccination in the country (CDC, 2022).
Linking HPV Vaccinations and Schools
A systematic review of medical literature by researchers at the Washington University School of Medicine revealed that school-based vaccination programs improve HPV vaccination rates by providing increased vaccine access and the ability to reach a large population, agnostic of individual access to healthcare services.
- Rhode Island adopted its “Vaccinate Before You Graduate” program in 2001, which ensures every student has the opportunity to be fully vaccinated before high school graduation or before moving from middle school to high school. The state contracts with a mass immunizer that is enrolled in the state-supplied vaccine program and can hold events anywhere in the state to provide vaccines, including HPV vaccine, at every middle and high school. According to the 2021 America’s Health Rankings report, Rhode Island has the highest HPV vaccination rate in the U.S.
Additionally, vaccination requirements for school entry can be very effective at driving vaccination rates and protecting students, staff, and communities from vaccine-preventable diseases. States that allow limited exemptions to routine vaccinations, such as Mississippi and California, have higher vaccination coverage rates than do states that permit a wider range of exemptions. While few states require HPV vaccination for school entry, other adolescent vaccination requirements, such as those for meningococcal vaccines, provide additional touch points between adolescent patients and their medical providers and increase opportunities to discuss and administer HPV vaccinations.
- Hawaii, Rhode Island, and Virginia all have HPV vaccination requirements for entry to 6th or 7th
- Vaccination rates among 11- to 12-year-old students rose 54 percent in 2019 after Puerto Rico implemented its school HPV vaccination requirement in 2018.
- While Mississippi does not require students to receive meningococcal or HPV vaccines for school entry, it has employed an opt out process for those vaccines. Parents are counseled on the importance of protecting their children with these vaccines and that HPV vaccine prevents cancer. Parents are then asked to sign a form if they do not want their child to receive the vaccines. As a result, HPV vaccination rates improved from 0.45 HPV vaccine for every Tdap vaccine in 2018 to 0.71 HPV vaccines for every Tdap vaccine in 2019.
Increase Access Through Pharmacist Administration
Forty-eight states, the District of Columbia, and Puerto Rico allow pharmacists to administer HPV vaccinations. However, according to unpublished data from the CDC, fewer than 120 pharmacies currently participate in the Vaccines for Children (VFC) program, a public program which provides vaccines at no charge to more than half of all children under age 18 years in the U.S. While many states have attempted to enroll pharmacies in the VFC program, nearly half of the enrolled pharmacies are located in in just two states. States can significantly impact HPV vaccine availability, especially in underserved areas, by recruiting pharmacists to the VFC program; however, pharmacists report several barriers to their participation including inadequate Medicaid payments for vaccine administration fees and complex VFC program requirements for vaccine inventory, storage, handling, and reporting. Identifying ways to overcome these challenges could have a positive impact upon not only HPV vaccination coverage rates, but those of several other recommended routine childhood and adolescent vaccines.
Allow Adolescent Consent
Most states allow emancipated minors to consent for their own medical care, but eight states (Alabama, Alaska, California, Delaware, Idaho, New York, Oregon, and South Carolina) and Washington D.C. allow adolescents to consent for HPV vaccination without a parent. According to an analysis of National Immunization Survey — Teen data, there was significant positive correlation between allowing adolescents to consent for HPV vaccination and HPV vaccine series initiation.
Recommend Earlier Administration of First Dose
While the CDC-recommended childhood immunization schedule routinely recommends HPV vaccination for boys and girls beginning at age 11, AAP recommends the vaccine series be started between ages 9 and 12 years. Starting early provides the ability to complete the two-dose vaccine series before other vaccines are given at age 11 years. A retrospective study showed adolescents who started the HPV series at age 9 or 10 were 22 times more likely to complete the series by age 15 years than those who started the series at age 11 or 12. State officials can provide education and recommendations to providers to begin the HPV vaccine series at ages 9 or 10 years and ensure public programs are aligned with those recommendations.
Utilize Immunization Information System (IIS) Functionality and Optimize Data Quality
All 64 states, large cities and U.S. territories that have immunization programs funded by the CDC use an IIS to record administered immunizations. Prior to the COVID-19 pandemic, funding for, and prioritization of, operational, data quality, and technology needs were lacking. States may consider using new federal funding streams to support core IIS functionality, including interoperability, data quality, and data access, which can help support HPV vaccination efforts.
- Reminder/Recall Tools
- A 2019 survey from the Association of Immunization Managers (AIM) revealed that only 37.7 percent of responding immunization programs used their IIS to perform centralized reminder/recall functions. States or medical practices using data from the IIS to generate automatic reminders to patients who are eligible for HPV vaccine or who lack series completion have the potential to improve HPV immunization rates through the use of centralized reminder/recall.
- North Dakota worked with their cancer coalition to award mini-grants to practices interested in increasing HPV vaccination rates, which practices used to fund a variety of strategies, including reminder/recall efforts. Providers used data from the IIS to identify those who were eligible for their second and third doses and sent postcard reminders to families.
- A 2019 survey from the Association of Immunization Managers (AIM) revealed that only 37.7 percent of responding immunization programs used their IIS to perform centralized reminder/recall functions. States or medical practices using data from the IIS to generate automatic reminders to patients who are eligible for HPV vaccine or who lack series completion have the potential to improve HPV immunization rates through the use of centralized reminder/recall.
- Exchange data with Medicaid programs
- The same AIM survey revealed fewer than half of responding IIS programs exchanged data with their Medicaid program as of 2019. Providing Medicaid programs with access to IIS data allows those programs to directly engage their beneficiaries around the importance of HPV vaccination. A recent publication by the Duke Margolis Center for Health Policy and the National Academy for State Health Policy summarizes strategies for data exchange between state immunization and Medicaid programs.
- Louisiana, Washington and Michigan use IIS data for Medicaid quality improvement strategies, including identifying populations with low vaccination rates to help inform outreach to Medicaid enrollees via managed care organizations.
- The same AIM survey revealed fewer than half of responding IIS programs exchanged data with their Medicaid program as of 2019. Providing Medicaid programs with access to IIS data allows those programs to directly engage their beneficiaries around the importance of HPV vaccination. A recent publication by the Duke Margolis Center for Health Policy and the National Academy for State Health Policy summarizes strategies for data exchange between state immunization and Medicaid programs.
- Require universal reporting to the IIS
- Without universal reporting of vaccinations administered within a state or territory, vaccination coverage rates can only be estimated, and reminder/recall efforts cannot be comprehensive. The federal requirement that COVID-19 vaccinations be entered into IIS has the potential to improve overall immunization reporting, as many providers now report administered COVID-19 vaccinations directly to the IIS via an electronic interface. States can encourage providers to not only report COVID-19 vaccinations, but all administered vaccinations, to the IIS. Doing so will help to ensure that individuals who are not fully vaccinated against HPV are reminded to do so. According to 2021 America’s Health Rankings, five of the states in the top 10 for HPV vaccine coverage rates have mandatory reporting for all vaccinating entities: Rhode Island, Massachusetts, Vermont, North Dakota, and New York.
- Allow Consumer Access to Individual Immunization Histories
- A recent publication by the National Governors Association outlines key considerations for modernizing IIS. One such consideration is facilitating public access to immunization records. Several states, including California, Arizona, Louisiana, Maryland, Mississippi, North Dakota, Washington, and West Virginia, have established portals that allow individuals to access their immunization history and receive reminders for future vaccinations. Such access may be particularly helpful to young adults who may be uncertain about their HPV vaccination status.
Leverage New and Existing Partnerships
- Most states have statewide, regional, and/or local immunization coalitions that work to improve immunization rates through education, advocacy, and outreach. States can support and partner with these coalitions to scale efforts to increase HPV immunization rates. The national Immunization Action Coalition also has a library of resources available to states that may assist with their efforts.
- St. Jude Children’s Research Hospital has developed a robust HPV Cancer Prevention Program that is working with states to strengthen medical provider recommendations for HPV vaccination. St. Jude has several publicly available resources that states can use to help communicate the importance of HPV vaccination as well as comprehensive state policy report.
- Regional and state cancer coalitions can be strong partners in promoting the importance of HPV vaccination rates and can assist with gathering stakeholders, sharing messaging, and identifying best practices to improve HPV vaccination rates.
Increasing HPV vaccination rates is critically important to protecting against several types of HPV-related cancers. The COVID-19 pandemic has created barriers to the vaccination of many adolescents who will remain at-risk for these preventable cancers.
Additional Resources
States can find additional resources through the National HPV Vaccination Roundtable, the Centers for Disease Control and Prevention, the American Academy of Pediatrics’ HealthChildren.org site, The Children’s Hospital of Philadelphia’s Vaccine Education Center, and the American Cancer Society.



