In response to COVID-19, many states have implemented emergency measures to ensure that Medicaid and Children’s Health Insurance Program (CHIP) enrollees continue to have access to essential health services. States have submitted disaster relief state plan amendments (SPAs) to the Centers for Medicare & Medicaid Services (CMS) to suspend and revise policies that could prevent enrollees from maintaining coverage and accessing care during the public health emergency.
Disaster relief SPA templates for CHIP and Medicaid outline actions states can take, including adjusting eligibility requirements, waiving premiums and cost sharing for enrollees, and expanding benefits. Some states have also implemented a new option provided by the Families First Coronavirus Response Act to extend Medicaid eligibility to uninsured individuals to cover COVID-19 testing and related services.
As states await CMS approval of their SPAs, several state Medicaid and CHIP agencies have already communicated important policy changes to enrollees through their websites. These announcements, in conjunction with approved disaster relief SPAs, show the wide range of actions states are taking to maintain enrollment, minimize the financial burden on enrollees, and increase access to care during the emergency.
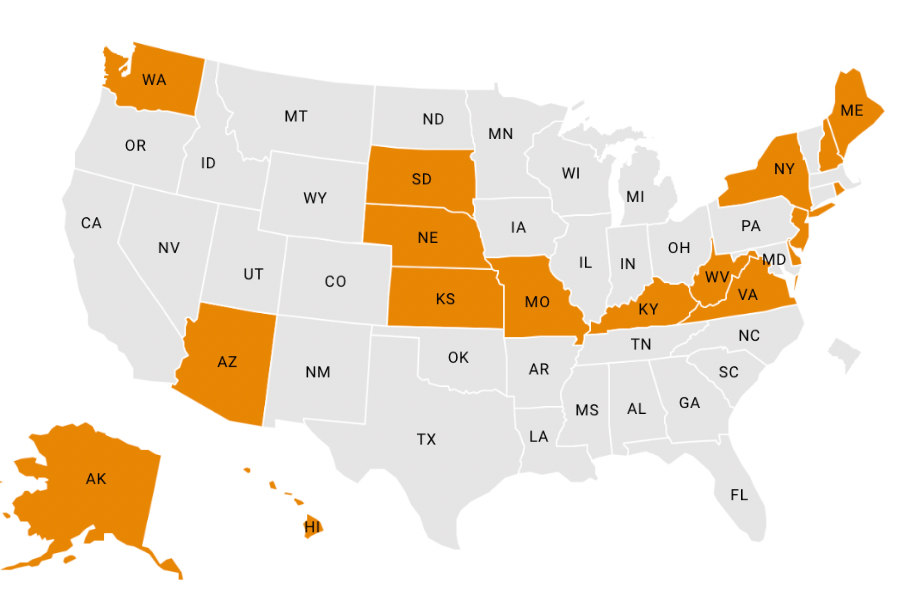
This chart describes the actions states have taken to protect and expand coverage for Medicaid and CHIP enrollees during the COVID-19 public health emergency, sourced from state websites and approved Medicaid and CHIP disaster relief SPAs.
Click on the state names to access relevant state documentation.
Support for this work was provided by the David and Lucile Packard Foundation. The views expressed here do not necessarily reflect the views of the foundation.