Executive Summary
State COVID-19 response relies on intensified cross-sector collaboration that supports timely, flexible, targeted action in the midst of quickly-changing circumstances. To provide insight into lessons learned at the state level, NASHP interviewed state officials from Illinois, Indiana, and Rhode Island about their states’ approaches to cross-agency COVID-19 response. This brief draws out key themes from these three states regarding:
- The role of leadership from governors;
- Best practices for engaging partners;
- The need for effective data systems;
- Approaches for using new and existing technology; and
- Strategies for leveraging new and existing funds, and centering equity.
| Theme | Key Take-aways |
| Leadership, Communication & Shared goals |
|
| Previously established partnerships |
|
| Community partnerships |
|
| Data-informed response |
|
| Improve data collection, management, & analytics |
|
| Center equity in the response |
|
| Technology and telehealth |
|
| New and existing funding sources |
|
Introduction and Background
The COVID-19 pandemic has offered major challenges and opportunities for state policymakers. Due to strained resources and rapidly changing circumstances, states have had to adapt quickly as they plan, coordinate, and manage services for residents. Several states established strong inter-agency partnerships to collectively facilitate cross-sector solutions in the immediate crisis. Public health, social service and other public sectors engaged in new ways with the health sector to address the range of health and social challenges and to strengthen the safety net. Some of this engagement leveraged cross-sector strategies already proliferating across the country to advance whole person health (including in rural communities)[1] and spurred efforts to address long-standing health inequities,ii especially in communities of color. This brief highlights Illinois, Indiana, and Rhode Island’s cross-agency strategies during COVID-19, and it draws out themes, lessons, and best practices for states to consider during recovery and when preparing for future public health emergencies.
There are clear benefits to cross-agency strategies in state government, and with a common direction, siloed approaches can give way to proactive collaboration. Barriers can include siloed budgets, limited data infrastructure, accountability structures for cross-cutting goals, and coordinated operations. Public health emergencies present a clear set of unifying goals, and cross-agency collaboration can be expedited—in part because governors in all states may declare a state of emergency, triggering a number of regulatory flexibilities, protections, and authorities to mobilize response.
COVID-19 emergency declarations and subsequent actions have created opportunities[2] to coordinate and align services across sectors to protect and restore individual health and well-being and build community resilience. This whole-of-government response activates coordination in crisis response and preparation for recovery. Early lessons suggest that successful cross-agency coordination rests on strong leadership, collaborative governance, a unifying strategic plan, aligned data tracking and sharing, increased state to local engagement, a priority focus on equity, and increased financial resources and flexibility through state and federal funding.
NASHP interviewed state officials from Illinois, Indiana, and Rhode Island who each work across various agencies to learn about their pandemic responses and how cross-agency collaboration played a role. Several key themes emerged in this midpoint analysis (see chart in executive summary for more detail on key themes):
Key Themes:
- Lead from the top with governors establishing direction, shared goals and mutual responsibility
- Engage partners to extend reach, bolster response, and increase equity – both previously established and new public, private partnerships at all levels of government and in communities
- Build effective data systems that allow actionable data sharing
- Use new and existing technology to leverage constituents’ needs and identify gaps in care
- Leverage new and existing funding to quickly resource effective and innovative initiatives
Leadership, Communication, and Shared Goals Can Break Down Silos and Make Unique Partnerships Possible
Key Points:
- Illinois Gov. Pritzker issued an Emergency Proclamation to mandate cross-agency partnerships between the Department of Health and the Emergency Management Agency
- Gov. Holcomb of Indiana set goals that created unique partnerships to help with PPE procurement and distribution.
- Rhode Island officials focused on using data to identify community needs, relying on existing Health Equity Zones (HEZs) to help meet those needs.
During the COVID-19 pandemic, governors became public faces of the pandemic response in their
states. States have always held[3] a unique role in emergency management, including their role to develop policy and governing strategy for public health preparedness. In all three states that NASHP interviewed, governors set goals for the pandemic response and recovery which helped to focus cross-agency efforts. Governors used their bully pulpit to raise awareness on the importance of timely pandemic response and rally their constituents and key stakeholders to respond. In particular, state officials noted that official communication structures set up to relay information to multiple agencies was key to ensuring cross-agency coordination and collaboration.
ILLINOIS
In Illinois, Gov. Pritzker issued an Emergency Proclamation[4] that facilitated and mandated cross-agency partnerships. It specifically called for coordination between the Illinois Department of Health and the Illinois Emergency Management Agency. When he took office, Gov. Pritzker set up a structure with four deputy governors who oversee agencies within their specific portfolio—budget and economy, education, public safety, and health and human services—in order to ensure efficient and coordinated government operations. This structure allowed for a more unified response to the pandemic (see figure 1). The governor regularly meets with these deputies to provide strategic direction and ensure operations are smooth. In addition, the Deputy Governor for Health and Human Services led a strategic planning process for her agencies before the pandemic began. The relationships formed during this process facilitated greater communication and collaboration in responding to the pandemic and implementing creative solutions to provide critical services even when public offices were closed.
Figure 1: Structure of Illinois’ COVID-19 Response in the Governor’s Office
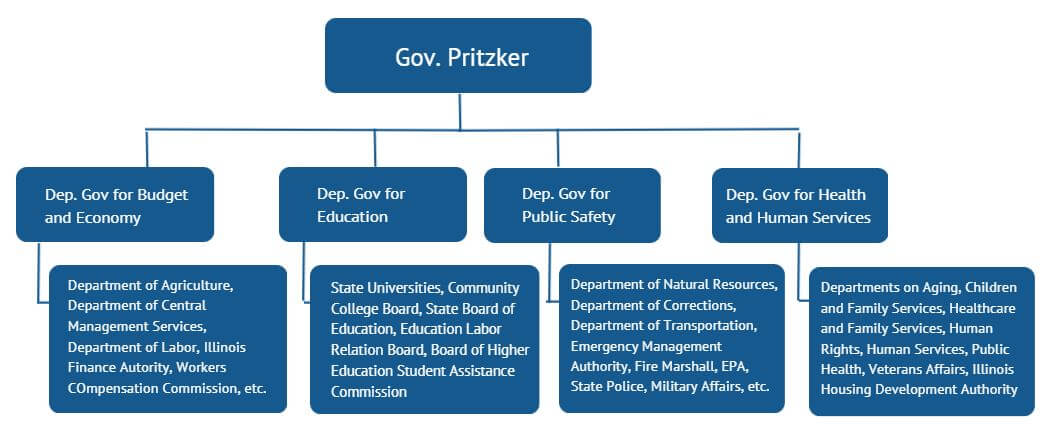
INDIANA
Similarly, an Indiana state official noted the Cabinet’s pre-existing, personal relationships established trust and strong communication pathways which helped state officials to identify and enhance cross-agency efforts and connections.
Collaboration was also driven by Gov. Holcomb’s dual priorities of pandemic response and economic recovery—both of which created the common goal of protecting workers and allowing businesses to safely remain open. Part of Indiana’s COVID-19 response, for example, was a partnership between Indiana’s Family and Social Services Administration (FSSA) and the Indiana Economic Development Corporation, the state’s economic development agency which acted as a personal protective equipment (PPE) procurement agency and PPE marketplace for small businesses.
RHODE ISLAND
Rhode Island routinely convenes multiple agencies to examine commonalities in their priorities and processes. For example, cross-agency work establishes and implements priorities for collaboration between Medicaid’s Accountable Entities and the Department of Health (RIDOH)’s Health Equity Zones (HEZs) to improve whole person care informed by community priorities.[5] HEZs are a unique partnership with local communities – supporting locally identified needs to build healthier, more resilient communities through a braided funding model. This unique existing infrastructure allowed for robust and swift state to local interaction, and prioritizing local needs.
Previously Established Partnerships Can “Grease the Wheels”
Key Points:
- In Illinois, existing cross-agency partnerships meant that staff were trained for pandemic responses prior to COVID-19.
- In Indiana, previously established academic partnerships, working partnerships in the Governor’s Cabinet, and the newly integrated 211 network were all reimagined for pandemic response.
- In Rhode Island, partnerships between state and local entities were critical for identifying needs and driving the response at the local, community level.
Every state official interviewed noted that they would not have been able to respond as readily to constituent needs during the pandemic without harnessing previously established relationships, both internally in their agency and externally across agencies.
ILLINOIS
Illinois officials noted the strong relationships between the Illinois Emergency Management Authority (IEMA), Illinois Department of Public Health (IDPH), and Department of Health and Human Services (DHHS). These agencies conducted many internal trainings and planning exercises leading up to the pandemic, which allowed them to respond more efficiently. The federal training “Crimson Contagion,”[6] conducted in 2019, had a direct correlation to the COVID-19 pandemic, and Illinois state officials noted this training was significant in helping plan their responses.
INDIANA
An Indiana state official noted that many of the systems put in place prior to the pandemic could be creatively leveraged during the pandemic response. For example, in 2019, Indiana entered into a contract that formed WISE[7]: a state-academic partnership between Medicaid and Indiana academic institutions that provides researchers with access to Medicaid data. The partnership was to officially begin in March 2020 but was stalled because of COVID-19. Instead, the partnership served as a research hub to inform Indiana’s science and evidence-based approach to the pandemic; every 12 hours researchers would conduct literature reviews to see what was happening across the state from a policy and science perspective, and this helped direct FSSA’s strategy and response.
Indiana’s established working partnerships across the Governor’s Cabinet became more important during the pandemic. For example, the cross-agency “My Healthy Baby”[8] program, to combat infant mortality among other initiatives, gave insight into the tools and resources that could be used in the pandemic.
RHODE ISLAND
Rhode Island officials noted the existing partnerships between school health and immunization departments was key in providing guidance for safe school re-opening. In Back 2 School Rhode Island, the Department of Health, the Department of Education, and the Local Education Agencies created a central hub of information to compile re-opening plans, school resources, and public health information. In addition, the state Medicaid program built on its relationship with the Department of Health for a more comprehensive pandemic response, including a variety of partners such as academic institutions and community-based organizations. In addition, Rhode Island’s HEZs were instrumental in building and maintaining trust for collective pandemic response. Although Rhode Island is a small state, it does not have local health departments, so the relationships between state officials, local leaders, mayors, and HEZ champions were key in identifying needs and driving response. Specifically, these partners supported and informed communities about the COVID-19 response, hosted pop-up testing sites and vaccination clinics in areas of high need, and facilitated feedback to state policymakers.
Community Partners Facilitate and Strengthen the Response
Key Points:
- In Illinois, specific communities were integrated into the response by embedding the health equity team into the broader COVID-19 response team.
- Indiana FSSA utilized the 211 network to identify individual needs and potential partners to help support those needs.
- Rhode Island’s HEZs were a critical resource and provided existing infrastructure to help identify needs and distribute resources to communities.
State official interviewed indicated that existing and newly formed community relationships, such as partnerships with community-based organizations and other local organizations like food pantries, federally qualified health centers (FQHCs) and other non-profit organizations were critical to building trust and disseminating information and resources.
ILLINOIS
On March 3, 2021, Illinois Governor Pritzker and the IDPH announced[9] a new partnership with four local FQHCs and five safety net hospitals to administer COVID-19 vaccines to residents in Cook, DuPage, and Lake Counties. IDPH also embedded the COVID-19 health equity team who worked with the state’s main COVID-19 response team to make sure that specific communities—including migrant farmworkers, houseless individuals, and those differently-abled were represented and included in pandemic response efforts.
INDIANA
The state 211 hotline, subsumed under FSSA’s purview just prior to the pandemic, was used early in the pandemic response to establish degree and location of needed wraparound services and case management for disease control and mitigation. The hotline became a critical tool for the agency to evaluate baseline needs in and connect with communities. FSSA staffed up the call line and added additional lines for other services, so that by the time vaccines became available, the department had around 1000 people answering calls. For example, the network received an influx of calls about food insecurity. After identifying this need, FSSA learned that food pantries were low on volunteers because their usual volunteer base was comprised of elderly individuals who were encouraged to stay isolated during the pandemic. FSSA partnered with the National Guard to fill this gap, deploying units to food pantries and achieving the extraordinary result of over 300 percent more food deliveries.
RHODE ISLAND
As in Illinois and Indiana, Rhode Island witnessed staggering and immediate needs (food and housing, most urgently) when the state instituted public health mitigation restrictions in March 2020. Non-profit partners experienced confusion about what services they could use grant funds for. In response, state officials spent several months working to clarify and change requirements and provide guidance. As HEZs brought new community organizations into the fold, Rhode Island’s community partners and network increased in coverage geographically by about 50 percent, totaling 15 HEZs covering 80 percent of the state during the pandemic. The HEZs were the “boots on the ground partners,” working to expand and scale the workforce at the community level by hiring over 200 community health workers[10] and other community outreach staff in two months. These community health workers carried out much of Rhode Island’s community-level work to address social needs exacerbated by the pandemic, like purchasing groceries for individuals in quarantine, helping newly eligible people apply for SNAP[11] benefits, delivering educational materials around pandemic safety, and conducting outreach about vaccines and administration of doses. Additionally, state officials mapped out community-based organizations tied to the COVID-19 response to create a hub-and-spoke model in which the HEZs served as the central fiduciary entities, dispensing funding to the community organizations. These strong community partnerships, with support from RIDOH, produced messaging about prevention, testing, vaccines, and more, helping to lower case rates in vulnerable communities.
Let the Data Drive and Inform the Response
Key Points:
- In Illinois, partnerships with local public health departments and hospitals, among others, provided data to help drive the pandemic response.
- Indiana’s previous efforts to facilitate data sharing and access by researchers made it easier to create functional data dashboards.
- Rhode Island used information gathered locally to drive targeted spending decisions.
Across states, officials interviewed emphasized reliance on data-driven, evidence-based policy decision-making to shape the state’s response to the pandemic. In particular, broader strategic planning for allocation of Coronavirus Aid, Relief, and Economic Security (CARES) Act dollars to maximize impact was informed by a variety of data sources.
ILLINOIS
In Indiana, data sharing was facilitated through pre-existing systems like the Management Performance Hub (MPH),[12] which was set up in 2014. Researchers used the MPH to access and manipulate data from across programs, including Medicaid, SNAP, TANF, and criminal justice. This resource made it easier to build COVID-19 data dashboards for internal and external use, and it also provided some needed context using previously collected social determinants of health data from SNAP questionnaires. Indiana’s integrated 211 network provided additional context for the kinds of social service supports people needed during the pandemic. The 211 network added real-time data, which helped to target interventions, like food supports, where they were most needed.
RHODE ISLAND
With information from community health workers (CHWs) and contact tracing/case investigation data, Rhode Island was able to tailor interventions to specific communities. Data analyses revealed the need to provide culturally appropriate food to people in quarantine and isolation in three communities hardest hit by the pandemic. HEZs provided the funding and the community created the mechanism to work with their case investigation/contact tracing team to deliver over 500,000 appropriate meals to people in quarantine. In another example, state officials saw a significant uptick in the number of people experiencing homeless in one of the poorest communities in the state. The HEZ reached out to RIDOH, which was able to provide significant financial resources, with limited restriction, to the HEZ to help provide mobile health and sanitation services, as well as emergency housing. Later in the response, this same hyper-local foundation of information drove what one state official described as “common-sense” vaccine distribution—prioritizing vaccine distribution[13] to vulnerable populations in Rhode Island first.
Continuously Improve Data Collection, Management, and Analytics
Key Points:
- All three states emphasized a need for more timely and complete data—which would require broad improvements to data collection and management.
- In Illinois, the state upgraded its public health data systems, and hospitals, the state health department, and local partners created new partnerships in order to compile and process COVID-19 data.
- In Indiana, COVID-19 necessitated an overhaul of data systems, and also an increase in state officials’ data literacy.
Having timely and complete data was critical for states’ responses. Officials from all three states emphasized the need for improved data collection and management systems. In particular, officials identified a clear need for robust, complete demographic data that can be disaggregated by key factors (such as race and ethnicity) to make strategic decisions[14] about how to address immediate and long-standing inequities.[15]
In Indiana, COVID-19 necessitated an overhaul of the state data systems and a renewed urgency around high quality, complete, and accurate demographic data. One change the state made was to make demographic data actionable by including more relevant options for racial and ethnic demographic information, thereby reducing use of “other.” An Indiana state official emphasized that the pandemic catalyzed a higher degree of data literacy across state government. With new priorities around data collection, disaggregation, analytics, and interoperability underpinning pandemic response along with new federal funding opportunities, states have a unique opportunity to build and enhance data systems that facilitate cross-agency collaboration in service of all communities.
Center Equity in the Response
Key Points:
- Illinois embedded a health equity team in the larger COVID-19 response team and started a Pandemic Health Navigators program to provide wrap-around services and help address barriers to effective quarantining or accessible care. Illinois also made additional efforts to reach the state’s rural population with rural outreach teams and mobile vaccination units.
- Indiana was one of several states to create new positions to help shape equity strategies across the whole-of-government.
- Rhode Island officials noted the need for a common understanding of what equity means and how different sectors can approach it.
The disproportionate COVID-19 burden in communities of color has effectively illuminated ongoing racial disparities across the United States. Some states have used cross-agency approaches to make the COVID-19 response more equitable and to better reach underserved communities who were disproportionately impacted by the pandemic.
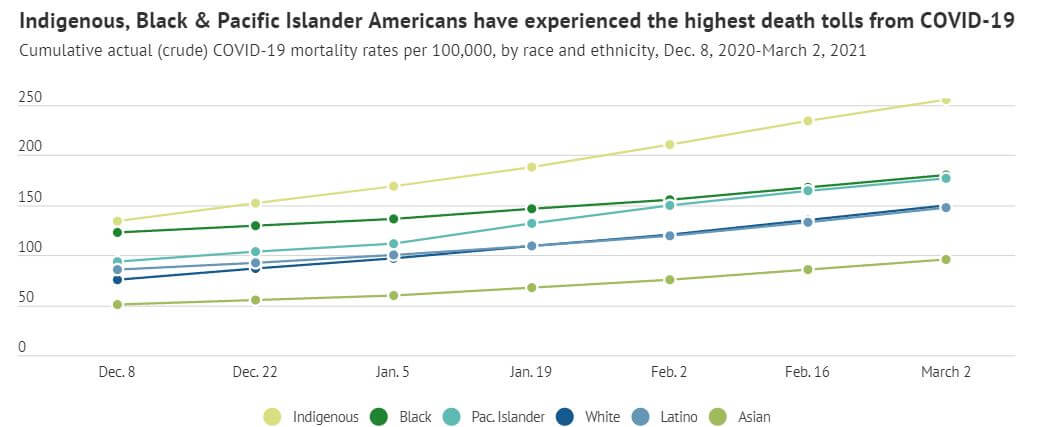
Population estimates from the U.S. Census Bureau, latest American Community Survey. Five-year estimates have been used for Indigenous and Pacific Islander rates, to improve data reliability.
Source: APM Research Lab Created with Datawrapper
The data states used to drive the COVID-19 response, including demographic and geographical information to track outbreaks and health and social factors and to target resources, illuminated ongoing racial health disparities across the country. The stark reality of these inequities, combined with the civil unrest during the summer of 2020, prompted an influx of new state strategies[16] to advance equity in the pandemic response and beyond. This work is ongoing. There are opportunities to build on state approaches, including federal leadership and resource allocation (e.g. funding[17] to support a community-based workforce and the federal COVID-19 health equity task force[18]) and an increase in public awareness of this issue, but also challenges, including political pressures and the need for sustainable financing, that states continue to grapple with.
ILLINOIS
Along with several other states, Illinois embedded a COVID-19 Health Equity team[19] in the wider COVID-19 response team. This group, which included community stakeholders and legislators, among others, was tasked with ensuring that specific communities were not left behind in the response. One approach that Illinois stood up was the Pandemic Health Navigator (PHN) program[20] which provided virtual health and wellness monitoring for people with COVID-19 in underserved communities. PHNs were a follow-on to the state’s successful contact tracing collaborative. PHNs provide wrap-around services to COVID positives and their close contacts to improve the odds of those persons maintaining isolation and quarantine, and PHNs were directed to ensure service in underserved communities. Since the program’s launch, the PHN program fulfilled over 6,700 resource requests across the state of Illinois. As is true in many states, Illinois residents experience barriers to care and services, such as lack of transportation, language, finances, technology or other existing illnesses – all exacerbated by the pandemic. The PHN program has created a robust network of locally-hired community health workers in both rural and urban communities. Due to their integration with the Illinois Contact Tracing Collaborative, this workforce is able to proactively reach out to those in need to assess their situation and connect them with resources to improve their ability to safely recover from, and prevent the spread of, COVID-19.
Throughout the pandemic response, Illinois also made additional efforts to reach its substantial rural population. A coordinated effort by IDPH, IEMA, and Illinois National Guard produced a vaccination effort that reached deep into the most rural areas of the state. This began early in the vaccination process as the National Guard deployed specifically designed “rural outreach teams” to different rural counties every day and provided vaccinations in areas of those counties with lower-than-average healthcare provider coverage. Further building on that success, IEMA and IDPH worked together to build a mobile vaccination group that was able to send out over 100 teams a week across the entire state to vaccinate wherever needed. These teams specifically targeted events like County fairs and food distributions in rural communities and were preceded on the ground by outreach teams trained by IEMA and IDPH to facilitate opportunities for rural populations to attend vaccination events. By designing solutions around the needs of rural communities and working in coordinated multi-agency fashion, Illinois was able to make significant progress against the unique vaccination challenges that rural communities face.
INDIANA
Indiana was one of several states that created new positions to help shape equity strategies across the whole of government. Gov. Holcomb hired a cabinet-level chief equity, inclusion, and opportunity officer, and FSSA hired a chief health equity and Americans with Disabilities Act (ADA) officer. The scope of these new positions goes beyond the pandemic response to try and address root causes of disparities. The cross-agency design[21] of these positions is meant to ensure that diversity, equity, and inclusion (DEI) efforts are not limited to one specific agency or sector. Rather, with the right funding and support, a person in this position will work across government agencies to advance equity and strengthen partnerships. A state official in Indiana noted that these partnerships improve the state’s ability to address the varying needs across geographies, disabilities or other barriers to achieving health equity.
RHODE ISLAND
Rhode Island’s HEZs operate with a common understanding of what equity is by lifting up individual community views on resources needed to engage and build a foundation for equitable change. The foundational work of arriving at common language, building interventions and funding mechanisms around an equitable, local approach through the HEZs was critical for centering equity and partnering with community members in the state’s pandemic response.
Technology and Telehealth Help Reach Vulnerable Communities
Key Points:
- Illinois and Rhode Island expanded telehealth flexibilities and officials in those states view telehealth as a successful tool to help improve access to care.
- Indiana introduced widespread telehealth options at the start of the pandemic, and saw a decrease in no-show rates. State officials are currently analyzing their data to identify ways to improve telehealth services in a more equitable way.
The COVID-19 pandemic became a catalyst[22] for states and the federal government to think about expanding access to healthcare and expanding telehealth services. Governors and other state officials used authorities like executive orders and Medicaid waivers as key levers to achieving this goal of identifying needs and caring for patients, especially vulnerable individuals and those in rural areas, who may not have previously had access to regular healthcare. Data showed[23] that older individuals and those living in rural communities experienced more challenges to health-related issues from COVID-19. Shifting delivery of medical services to telehealth was a key policy change to ensure these more vulnerable individuals’ and communities’ needs were met during the pandemic.
ILLINOIS
Illinois expanded telehealth flexibilities[24] in Medicaid during the pandemic, including around the site of service delivery and reimbursing for needed services such as behavioral health services using real-time audio-only telephone or video interactions, virtual check-ins, and online patient portal e-visits. To reach more people who were unable to access services, the state 1) established reimbursement rates for telehealth services equivalent for those offered face-to-face and 2) engaged provider and advocate partners to help communicate the availability of telehealth services to beneficiaries. In addition, the Governor issued an Executive Order requiring commercial insurers to reimburse health care providers for telehealth with the same payment rates as in-person care. Both efforts have now been made permanent through administrative rules and legislation. State officials working at the Illinois Housing Development Authority also noted that moving the agency’s housing portal online for residents increased the number of people who were able to access rental assistance.
INDIANA
Indiana had not previously used telehealth widely, but FSSA implemented telehealth flexibilities without exceptions through Medicaid at the beginning of the pandemic and learned very quickly about what worked and what did not. With 16 months of data, FSSA was able to identify trends and consider how telehealth could be used post-pandemic. For example, some community mental health centers reported seeing “no-show” rates go from as high 60 percent to less than 10 percent, demonstrating pent up demand for mental health services and/or pandemic-related access barriers. State officials also noted that racial and ethnic disparities in mental health service utilization widened during the pandemic–which will be a state and agency focus moving out of the pandemic. Flexibility with telehealth is a service area the legislature has made permanent, and FSSA continues to work towards achieving equity using the data they collected during the pandemic.
RHODE ISLAND
Rhode Island saw success in implementing flexibilities through telehealth and integrating data systems across agencies. Having a crosscutting view of the data allowed state officials to identify provider and patient use of telehealth and evaluate effectiveness. Data indicated that telehealth was effective in increasing identification and treatment of COVID patients and allowed the state to target high-need areas to place testing and vaccine clinics.
Leveraging New and Existing Sources of Funding to Amplify Response
Key Points:
- In Illinois, CARES Act funding supported a variety of work in different agencies, with some funds going directly to community partners and being used to improve specific aspects of the pandemic response including testing, tracing, and vaccination, where needed.
- Indiana FSSA used ARPA funding to create a separate business unit that will blend and braid existing funds with this one-time funding to support all of Indiana’s Human Services.
- Rhode Island state officials are thinking about the future of the state’s public health funding, including the future of quality and payment models for long-term services and supports.
States are using the influx of federal support to states during the pandemic through the CARES Act and American Rescue Plan Act (ARPA)[25] in a variety of ways. Cross-agency collaboration can promote cross-cutting investments to both shore up pandemic response and to find opportunities for sustainable, cross system approaches to improving resident’s health and well-being.
ILLINOIS
The Illinois Department of Healthcare and Family Services (HFS) received $700 million in the first round of CARES Act funding. HFS was able to use part of the funding to address gaps in care due to reduced use during the pandemic and to engage enrollees.
The Illinois’ Department of Human Services (DHS) used $60 million of its CARES Act first round of funding to directly support community organizations. DHS provided funding to childcare programs, providers, food banks, and to bring immediate relief to families. During the civil unrest that occurred in the summer of 2020, DHS funded young community members to help rebuild small businesses and to support community colleges to ensure young people could continue online learning. DHS also funded public relations firms to conduct public education and build awareness about the availability of testing and COVID-19 precautions among people of color. This included investment in faith-based institutions as key messengers. With CARES Act funding, DHS also worked with the Department of Commerce and Economic Opportunity to create the Child Care Restoration Grants,[26] and this model was used to inform the federal ARPA childcare stabilization grants. The program began providing grants on a quarterly basis starting in July 2020, and continues to provide grants to licensed childcare centers, licensed family childcare, and license-exempt centers. DHS also leveraged CARES Act funding in 2020 to expand childcare assistance for health care sector employees, emergency responders, sanitation and other essential workers.
IDPH received $300 million for contact tracing at the local health department level and funded wraparound services for quarantine and isolation. Building up the state’s testing network also required significant financial commitment, including upgrading data collection and management systems and increasing workforce capacity, all with the goal of addressing the current pandemic while making sure Illinois is prepared for any future crises.
INDIANA
Indiana received approximately $3 billion in ARPA funds. FSSA had many conversations around how to use this one-time funding in creative and sustainable ways to assist the recovery process without creating a difficult situation when the funds run out. FSSA created a separate business unit with ARPA funding to support all of Indiana Human Services by blending and braiding funds with this one-time funding. One use for the dollars might be mental health care network evaluation— looking at how to expand the workforce pipeline, how to ensure the use of evidence-based care, and how to improve telehealth. Indiana is also looking into infrastructure supports with this funding, including activities like helping to support health improvements in childcare facilities such as lead assessment and abatement. The agency is looking for ways to identify pilots that are scalable. However, while the public health emergency continues, and people are still getting sick and needing financial assistance, FSSA will use some additional funding for Medicaid eligibility vouchers, helping to eliminate copays and assisting families through this emergency. Indiana also expanded[27] postpartum Medicaid coverage to 12 months, and this benefit will start as soon as the public health emergency ends.
RHODE ISLAND
Rhode Island used federal funding for both preventive and stop-gap measures. For example, because Medicaid pays for half of long-term care and congregate care facilities that were “absolutely ravaged” during the pandemic, state officials predicted this will have long-term budget implications for the entire Medicaid program. State officials also noted the unique opportunity to rethink quality and payment models for long-term services and supports. Federal assistance[28] through the 10 percent Federal Medical Assistance Percentages (FMAP) payment increase and ARPA funds will also support rebuilding, but the state noted the limited time frames to spend the funds, and significant fiscal damage from the pandemic challenge a sustained strategic investment approach. For example, the state’s Part C Early Intervention referral rates were down around 20 percent, with huge disparities in follow up; the impact of this decrease will stretch far beyond March 2024. Further, they expressed a concern that the public health systems nationwide have been chronically underfunded and investments are needed to modernize a collaborative public health response to this and similar crises.
Conclusion: The Necessity of Addressing this Crisis Together
In a crisis of this magnitude, it was impossible for any single agency to address the work alone, and states saw success when they were able to draw from and strengthen existing partnerships or build new partnerships with unlikely allies. However, state officials cautioned a too swift return to normalcy—they noted that while partners were quick to break out of their individual silos, they were also quick to return to them. And the pandemic is not over; as states transition from a state of emergency to living with the virus and the ever-evolving nature of its variants, maintaining these partnerships will remain critical. Several states are in the process of evaluating pieces of their COVID-19 response. Lessons learned, key takeaways, and newly identified challenges will continue to emerge as states conduct evaluations—all of which will be crucial for addressing COVID-19 as a constant, as we move to recovery and in preparing for the next emergency.
End Notes
[1] Landers, G. et. Al, (2020, August). “Finding Innovation and Resilience During the COVID-19 Pandemic: Cross-Sector Alignment and the Response to COVID-19.” Georgia Health Policy Center. https://ghpc.gsu.edu/2020/08/07/cross-sector-alignment-and-the-response-to-covid-19/.
[2] Landers, G. et. Al, (2020, August). “Finding Innovation and Resilience During the COVID-19 Pandemic: Cross-Sector Alignment and the Response to COVID-19.” Georgia Health Policy Center. https://ghpc.gsu.edu/2020/08/07/cross-sector-alignment-and-the-response-to-covid-19/.
[3] National Governors Association. Virtual Resource Center for Public Health Emergency Preparedness. https://www.nga.org/public-health-preparedness-resource-center/.
[4] State of Illinois Executive Department, Gubernatorial Disaster Proclamation. (2021, February). https://www2.illinois.gov/sites/gov/Documents/CoronavirusDisasterProc-2-5-2021.pdf.
[5] Rhode Island Department of Health. “Health Equity Zones: Building healthy and resilient communities across Rhode Island.” https://health.ri.gov/publications/brochures/HealthEquityZones.pdf.
[6] U.S. Department of Health and Human Services, Office of the Assistant Secretary for Preparedness and Response. “Crimson Contagion 2019 Functional Exercise After-Action Report.” (2020, Jaunary). https://www.governmentattic.org/38docs/HHSaarCrimsonContAAR_2020.pdf.
[7] Indiana Clinical and Translational Sciences Institute. WISE Indiana (Wellbeing Informed by Science and Evidence in Indiana). https://indianactsi.org/community/monon-collaborative/wise-indiana/.
[8] Indiana Department of Health, Family and Social Services Administration, and Department of Child Services. My Healthy Baby. https://www.myhealthybabyindiana.com/.
[9] Office of Gov. J.B. Pritzker. “Press Release: State Partners with Local Hospitals and Health Centers to Expand Equitable Distribution of Vaccine in Cook and Collar Counties.” (2021, March). https://www.illinois.gov/news/press-release.22880.html.
[10] State of Rhode Island Department of Health. Community Health Workers. https://health.ri.gov/communities/about/workers/.
[11] State of Rhode Island Department of Human Services. Supplemental Nutrition Assistance Program (SNAP): Eligibility and How to Apply. https://dhs.ri.gov/programs-and-services/supplemental-nutrition-assistance-program-snap/supplemental-nutrition-0.
[12] Indiana Management Performance Hub (MPH). Enhanced Research Hub. https://www.in.gov/mph/projects/enhanced-research-environment/.
[13] Rhode Island Department of Health COVID-19 Information. Rhode Island’s Hard-Hit Community Vaccination Strategy. https://covid.ri.gov/vaccination/rhode-islands-hard-hit-community-vaccination-strategy.
[14] Higgins, E., (2020, October). “States Work to Advance Racial Equity in COVID-19 Outcomes and Beyond.” National Academy for State Health Policy. https://www.oldsite.nashp.org/states-work-to-advance-racial-equity-in-covid-19-outcomes-and-beyond/.
[15] Zylla, E. et. Al, (2021, June). “Ensuring Equity: State Strategies for Monitoring COVID-19 Vaccination Rates by Race and Other Priority Populations.” State Health & Value Strategies. https://www.shvs.org/ensuring-equity-state-strategies-for-monitoring-covid-19-vaccination-rates-by-race-and-other-priority-populations/.
[16] National Academy for State Health Policy. “How States Collect, Report, and Act on COVID-19 Race and Ethnicity Data.” https://www.oldsite.nashp.org/how-states-report-covid-19-data-by-race-and-ethnicity/#tab-id-2.
[17] U.S. Department of Health and Human Services. “HHS Awards $125 Million in Workforce Grants for Community-Based Efforts to Bolster COVID-19 Vaccinations in Underserved Communities.” (2021, June). https://www.hhs.gov/about/news/2021/06/14/hhs-awards-125-million-in-workforce-grants-to-bolster-covid-19-vaccinations-in-underserved-communities.html.
[18] U.S. Department of Health and Human Services Office of Minority Health. About COVID-19 Health Equity Task Force. https://www.minorityhealth.hhs.gov/omh/browse.aspx?lvl=2&lvlid=100.
[19] Illinois Department of Public Health. COVID-19 Health Equity Task Force. https://www.dph.illinois.gov/covid19/health-equity-task-force.
[20] Illinois Department of Public Health. COVID-19 Pandemic Health Navigator Regional Coordinators. https://www.dph.illinois.gov/rfp/covid-19-pandemic-health-navigator-regional-coordinators.
[21] Atkeson, A. (2021, February). “State Policy and Program Strategies to Advance Health and Racial Equity.” National Academy for State Health Policy. https://www.oldsite.nashp.org/state-policy-and-program-strategies-to-advance-health-and-racial-equity/#tab-id-1.
[22] National Governors Association. “The Future of State Telehealth Policy.” (2020). https://www.nga.org/wp-content/uploads/2020/11/The-Future-of-State-Telehealth-Policy.pdf.
[23] Henning-Smith, C. (2020, May). “The Unique Impact of COVID-19 on Older Adults in Rural Areas.” Journal of Aging and Social Policy, Vol. 32: 4-5, 396-402. https://www.tandfonline.com/doi/full/10.1080/08959420.2020.1770036.
[24] Department of Healthcare and Family Services. “Notice of Emergency Ammendment, Title 89: Social Services.”https://www2.illinois.gov/hfs/SiteCollectionDocuments/03202020TelehealthAmendments89140RGE.pdf.
[25] U.S. Congress, House, American Rescue Plan Act of 2021, HR 1319, 117th Cong., introduced in House February 24, 2021. https://www.congress.gov/bill/117th-congress/house-bill/1319/text.
[26] Gateways to Opportunity, Illinois Professional Development System. Childcare Restoration Grants. https://www.ilgateways.com/financial-opportunities/restoration-grants.
[27] Smith, B. (2021, April). “Indiana Expanding Medicaid Coverage To New Mothers 12 Months Postpartum.” WFYI Indianapolis. https://www.wfyi.org/news/articles/indiana-expanding-medicaid-coverage-to-new-mothers-12-months-postpartum.
[28] Chidambaram, P. & Musumeci, M. (2021, May). “Potential Impact of Additional Federal Funds for Medicaid HCBS for Seniors and People with Disabilities.” Kaiser Family Foundation. https://www.kff.org/medicaid/issue-brief/potential-impact-of-additional-federal-funds-for-medicaid-hcbs-for-seniors-and-people-with-disabilities/.
This project is supported by the Health Resources and Services Administration (HRSA) of the US Department of Health and Human Services under grant number U2MOA394670100, National Organizations of State and Local Officials. This information, content, or conclusions are those of the authors and should not be construed as the official position or policy of, nor should any endorsements be inferred by HRSA, HHS or the US government.
The authors would also like to thank the state officials in Rhode Island, Illinois, and Indiana for providing content and review, and the work they are doing in their states to address the pandemic, as well as their colleagues at NASHP for their review and insights.




