Updated September 28, 2020
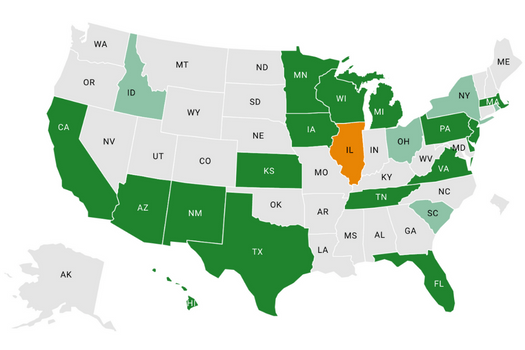
Absent a pandemic, enrollees usually sign up for insurance coverage during the annual open enrollment period, from Nov. 1- Dec. 15. However, under extenuating circumstances, consumers can sign up during a special enrollment period (SEP). The Affordable Care Act defined a set of events that trigger SEPs nationally (view a national list of SEPs), but state-based marketplaces have limited discretion over when to schedule additional SEPs for their consumers. Many have enacted SEPs in response to the COVID-19 pandemic to give uninsured residents an opportunity for coverage, which reduces financial barriers in the event they need medical care. Below is a list of the unique SEPs available in state-based marketplaces, including life-changing events, unexpected health plan changes, or enrollment in dental coverage.
| What Events Qualify for a Special Enrollment Period in State-Based Marketplaces | |||||||||||||
| Qualifying Event | CA | CO | CT | DC | ID | MD | MA | MN | NV | NY | RI | VT | WA |
| Special Enrollment Periods (SEPs) triggered by unique life events: | |||||||||||||
| Loss of coverage upon leaving military service | x | ||||||||||||
| Loss of “hardship exemption” (exemption from individual mandate penalty) | x | x | x | x | |||||||||
| A change in disability status | x | x | |||||||||||
| Pregnancy (self-attested or requiring verification) | x | x | x | x | x | ||||||||
| Newly eligible for state coverage because of change in income | x | ||||||||||||
| Beginning or end of state hardship waiver that reduces or waives premiums | x | ||||||||||||
| SEPs triggered due to insurance market changes: | |||||||||||||
| Health insurance plan became decertified during the coverage year | x | x | |||||||||||
| Provider left health plan network while enrollee was receiving care or treatment for illness | x | ||||||||||||
| SEPs due to eligibility/ reconciliation issues: | |||||||||||||
| Was conditionally approved for Medicaid during open enrollment period (OEP) or SEP, but was ultimately denied and received denial notice after the OEP/SEP ended | x | x | x | x | |||||||||
| Enrollee was automatically renewed into a different plan without forewarning because original plan was no longer offered | x | ||||||||||||
| Consumer’s employer was going to enroll employees in SHOP coverage, but was denied because too few employees selected coverage | x | ||||||||||||
| Tax filer learned of state/district individual mandate during tax season or was assessed a tax penalty through the mandate | x | x | x | ||||||||||
| SEPs due to technical issues or extenuating circumstances: | |||||||||||||
| SEP triggered for victims of a natural disaster (ex., wildfires). | x | ||||||||||||
| Loss of coverage due to the failure of a provider/provider-funded third party to pay enrollee’s premium on a timely basis (effective 7/1/2020) | x | ||||||||||||
| Termination of coverage caused by a problem with automatic payment (e.g., because credit card was discontinued because of fraudulent activity) | x | x | |||||||||||
| Acts of foreign or domestic terror prevented enrollee from meeting enrollment deadlines | x | x | |||||||||||
| SEP triggered in the event of a public health emergency* | x | x | x | x | x | x | x | x | x | x | x | x | |
| Customer’s enrollment issue (non-system error) was not resolved before the end of OEP | x | x | x | x | |||||||||
| SEPs triggered by fraudulent coverage: | |||||||||||||
| Purchased fraudulent coverage policy through Simple Health insurance company (temporary; expired) | x | x | x | x | x | x | x | ||||||
| Bought other fraudulent coverage (e.g., coverage that misrepresented itself as comprehensive coverage) | x | ||||||||||||
| Member of Aliera “health-sharing ministry” and wished to switch to comprehensive plan (temporary; expired) | x | x | |||||||||||
| SEPs for enrollment in dental plan: | |||||||||||||
| Consumer is newly eligible for Medicaid or qualified health plan, enrolled in SHOP, or gained access to an excepted benefits health reimbursement arrangement and otherwise lacks dental coverage | x | ||||||||||||
| Open SEP to purchase dental coverage | x | ||||||||||||
| Loss of other dental coverage | x | ||||||||||||
Updated September 28, 2020
*Time-limited SEPs created in response to the COVID-19 national emergency. These SEPs are/were open during the following periods.
CA 3/20/20 – 8/31/20
CO 3/20/20 – 4/30/20
CT 3/19/20 – 4/17/20
DC 3/18/20 – 9/15/20
MD 3/16/20 – 7/15/20; 8/7/20-12/15/20
MA 3/11/20 – 5/25/20
MN 3/23/20 – 4/21/20
NV 3/17/20 – 5/15/20
NY 3/16/20 – 9/15/20
RI 3/14/20 – 4/30/20
VT 3/20/20 – 6/15/20
WA 3/09/20 – 5/08/20